1. PCOD Treatment: Understanding Polycystic Ovary Disorder

PCOD Treatment Guide – Topics Covered
This comprehensive PCOD guide explains symptoms, causes, lifestyle management, diet strategies, fertility considerations and treatment options. Use the table of contents below to navigate different sections.
Table of Contents
- Understanding PCOD
- How the Ovaries Work in a Normal Menstrual Cycle
- What Happens in PCOD: Understanding the Hormonal Mechanism
- PCOD vs PCOS: Understanding the Difference
- Why PCOD Happens: Root Causes and Risk Factors
- Common Symptoms of PCOD
- PCOS Lifestyle Self-Evaluation Tool
- PCOS Lifestyle & Symptom Self-Evaluation Tool
- Lifestyle Changes That Help Manage PCOD
- Weekly PCOS Lifestyle Planner
- PCOD Diet Planning and Hormonal Nutrition
- PCOS Friendly Food Explorer
- PCOD and Weight Gain
- PCOD and Fertility
- Medical Treatment Options for PCOD
- Scientific Research and Medical Evidence on PCOD
- When Should You See a Doctor for PCOD?
- Long-Term Health Risks of Untreated PCOD
- Frequently Asked Questions
What is PCOD
Polycystic Ovary Disorder, commonly known as PCOD, is one of the most frequently diagnosed hormonal conditions affecting women in their reproductive years. Many women first become aware of PCOD when they begin experiencing irregular menstrual cycles, delayed periods, persistent acne, weight gain or unexpected hormonal symptoms. Others may discover the condition later when they start investigating fertility challenges. Because the symptoms can vary widely from one person to another, PCOD is sometimes misunderstood or diagnosed late.
Hormonal Communication and Ovarian Function
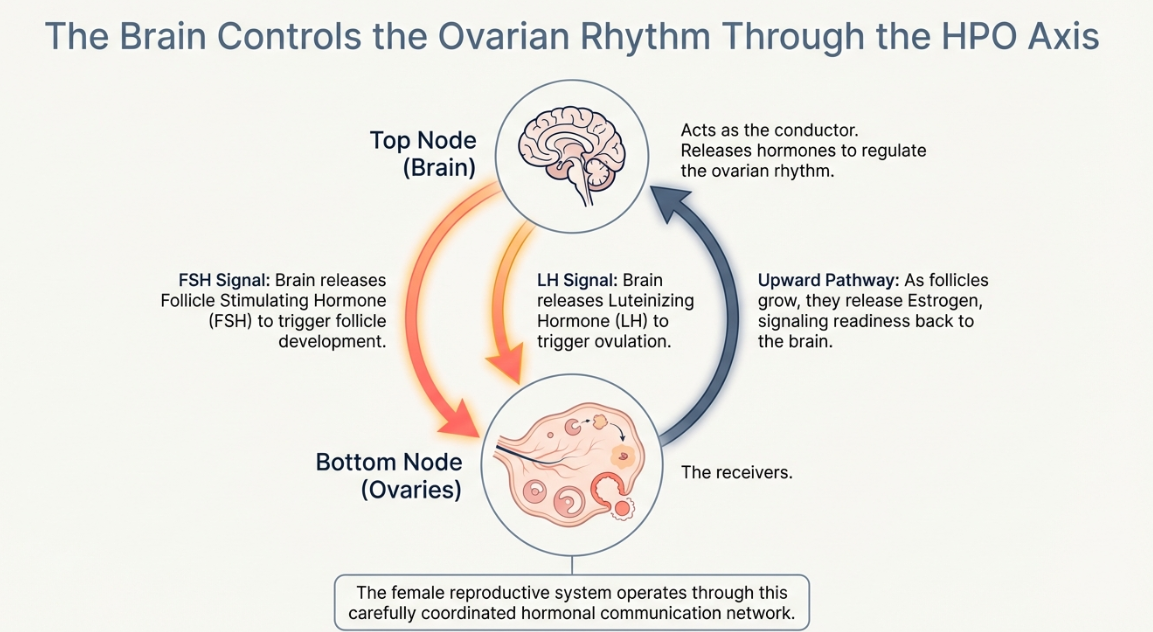
PCOD is not simply an ovarian problem. It is a complex hormonal and metabolic condition that affects how the ovaries, endocrine system and metabolism interact with each other. Hormones released from the brain communicate with the ovaries to regulate ovulation and the menstrual cycle. In PCOD, this delicate hormonal communication becomes disrupted. As a result, ovulation may occur irregularly or not occur at all, which can lead to multiple immature follicles developing within the ovaries and irregular menstrual cycles.
Symptoms and Health Effects of PCOD
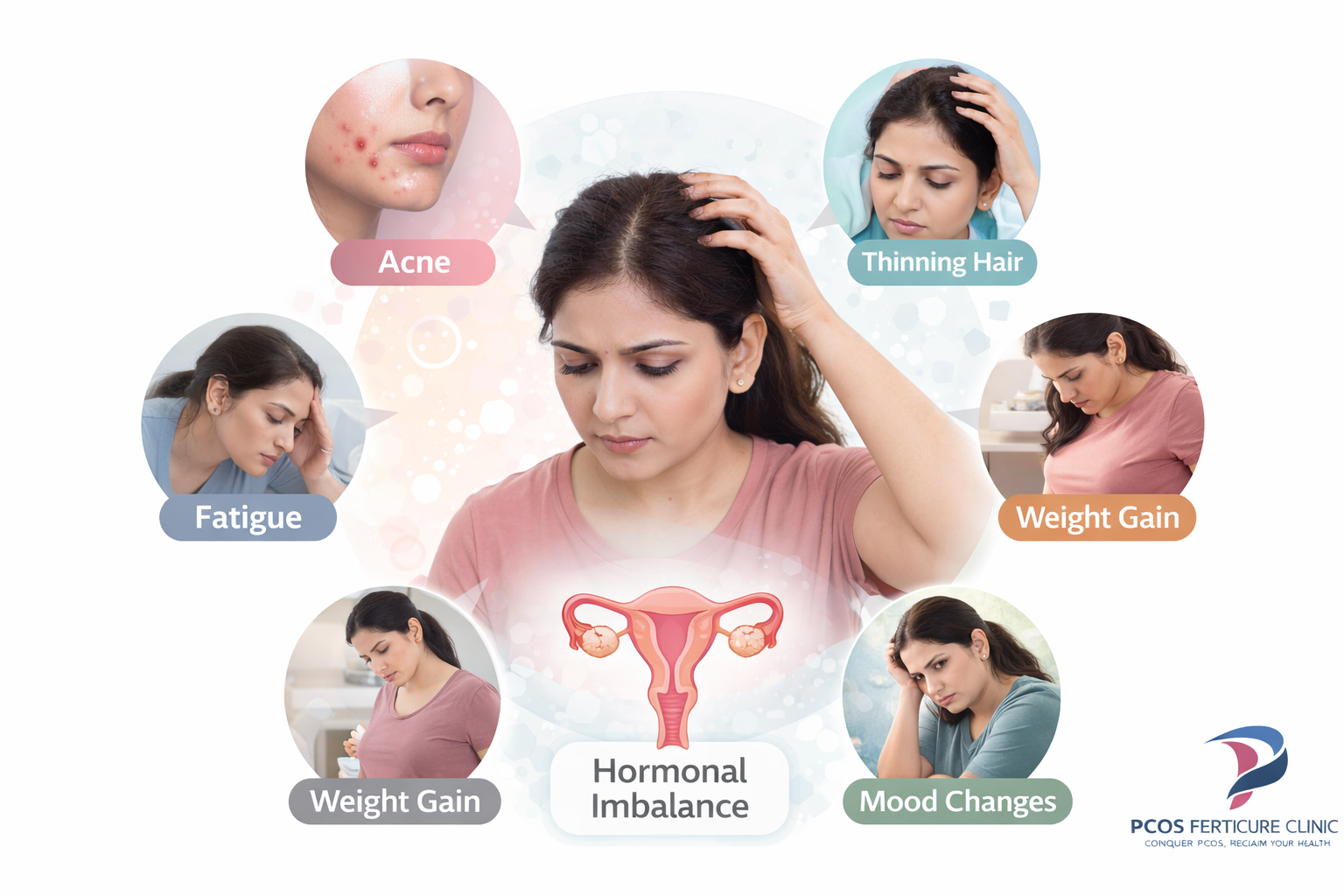
Hormonal imbalance associated with PCOD can influence several areas of health. Women may experience symptoms such as acne, increased facial hair, scalp hair thinning, fatigue, weight gain, mood fluctuations or difficulty maintaining regular cycles. Some women experience only mild symptoms while others may develop a broader pattern of metabolic and hormonal changes over time. Because of this variability, treatment approaches for PCOD usually focus on understanding the underlying hormonal pattern and managing the condition gradually rather than relying on a single quick solution.
Diagnosis and Medical Evaluation
Understanding how PCOD develops is the first step toward effective management. Diagnosis typically involves reviewing menstrual history, evaluating symptoms and performing hormonal tests or ultrasound examination when needed. If you would like to understand how doctors evaluate this condition, you can read our detailed guide on PCOS diagnosis where we explain common diagnostic tests and medical criteria used in clinical practice.
Lifestyle and Metabolic Factors in PCOD
Many women with PCOD also notice changes in their metabolism, particularly difficulty managing weight. Hormonal imbalance and insulin resistance can influence how the body stores fat and processes carbohydrates. For this reason, lifestyle strategies such as nutrition planning, physical activity and metabolic health management are often important parts of treatment. You can explore practical approaches on our PCOS weight loss guide, which explains why weight regulation can be challenging in PCOD and how it can be improved safely.
Role of Diet in Hormonal Balance
Diet also plays a significant role in supporting hormonal balance. Certain eating patterns can help stabilize blood sugar levels, reduce inflammation and support better metabolic health. If you want to understand which foods are commonly recommended for women with hormonal imbalance, our PCOD diet chart explains how balanced meals can support long-term management of PCOD symptoms.
Role of Diet in Hormonal Balance
Because PCOD influences both reproductive and metabolic health, many women also worry about future fertility. The good news is that many women with PCOD conceive successfully once ovulation patterns are understood and hormonal balance improves. If fertility is one of your concerns, you may find our article on PCOS fertility management helpful in understanding how ovulation and conception are supported in women with hormonal imbalance.
What This Guide Will Help You Understand
This page serves as a comprehensive guide explaining how PCOD develops, what symptoms may appear, how diagnosis works and what treatment strategies are commonly used to manage the condition. As you read further, you will also find practical lifestyle guidance and interactive tools that can help you better understand your hormonal health and explore personalized management strategies.

2. How the Ovaries Work in a Normal Menstrual Cycle
Hormonal Communication Between Brain and Ovaries
To understand PCOD properly, it is important to first understand how the ovaries normally function during a menstrual cycle. The female reproductive system operates through a carefully coordinated hormonal process known as the hypothalamic-pituitary-ovarian axis. In this system, the brain communicates with the ovaries using hormones that regulate follicle development, ovulation and menstrual cycles.
Follicle Development and Egg Maturation
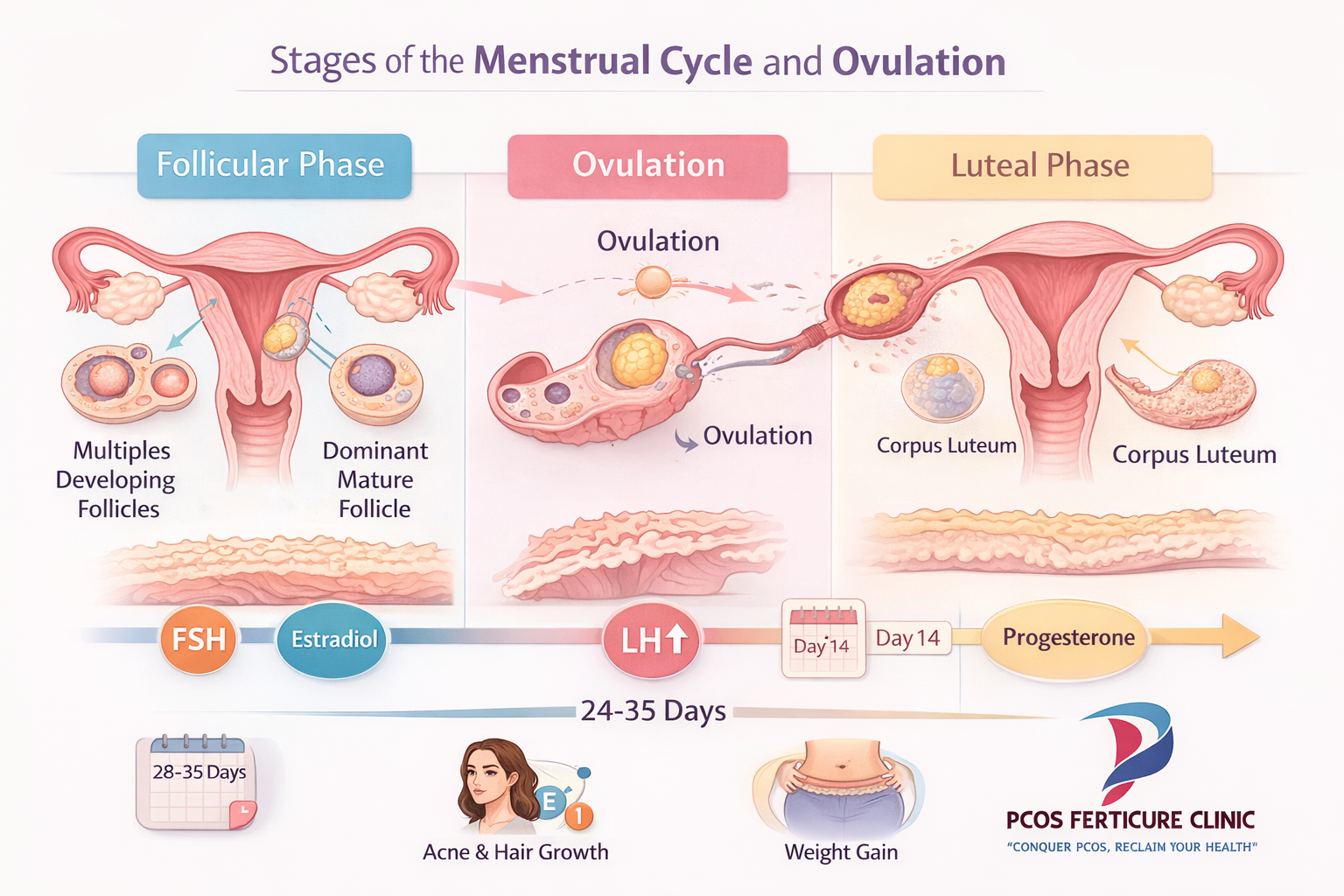
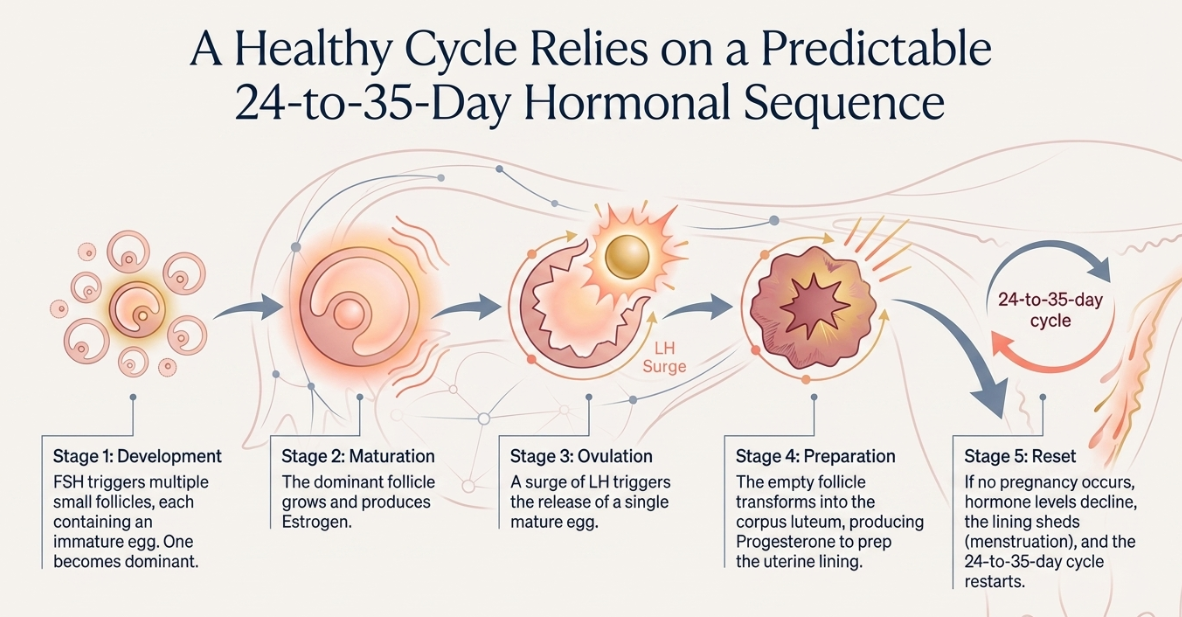
At the beginning of each menstrual cycle, the brain releases follicle stimulating hormone (FSH). This hormone signals the ovaries to begin developing multiple small follicles. Each follicle contains an immature egg. During the early part of the cycle, several follicles may start growing, but usually one follicle becomes dominant and continues to mature.
As the dominant follicle grows, it produces estrogen. Rising estrogen levels signal the brain that the follicle is ready for ovulation. The brain then releases another hormone called luteinizing hormone (LH). A surge of LH triggers ovulation, which means the mature egg is released from the ovary and becomes available for fertilization.
Ovulation and Hormonal Rhythm
After ovulation occurs, the follicle transforms into a structure known as the corpus luteum. This structure produces progesterone, a hormone that prepares the lining of the uterus for possible pregnancy. If pregnancy does not occur, hormone levels gradually decline and the uterine lining sheds, resulting in a menstrual period. The cycle then begins again.
In women with regular cycles, this process typically occurs every 24 to 35 days. Hormones rise and fall in a predictable rhythm, ovulation happens once during each cycle and the ovaries release a mature egg regularly. This hormonal rhythm is essential not only for fertility but also for maintaining overall reproductive health.
What Happens When Ovulation Does Not Occur
However, when the hormonal communication between the brain and ovaries becomes disrupted, ovulation may not occur consistently. This disruption is exactly what happens in conditions such as PCOD and PCOS. Instead of one follicle maturing and releasing an egg, several follicles may stop developing midway. These immature follicles may accumulate in the ovary, which is why ultrasound scans sometimes show multiple small follicle structures in women with hormonal imbalance.
Understanding the normal ovulation cycle makes it easier to understand why PCOD leads to irregular periods, delayed cycles and hormonal symptoms. In the next section, we will explore what exactly changes inside the ovaries when PCOD develops and how hormonal imbalance alters the ovulation process.
3. What Happens in PCOD: Understanding the Hormonal Mechanism
Disruption of the Normal Ovulation Process
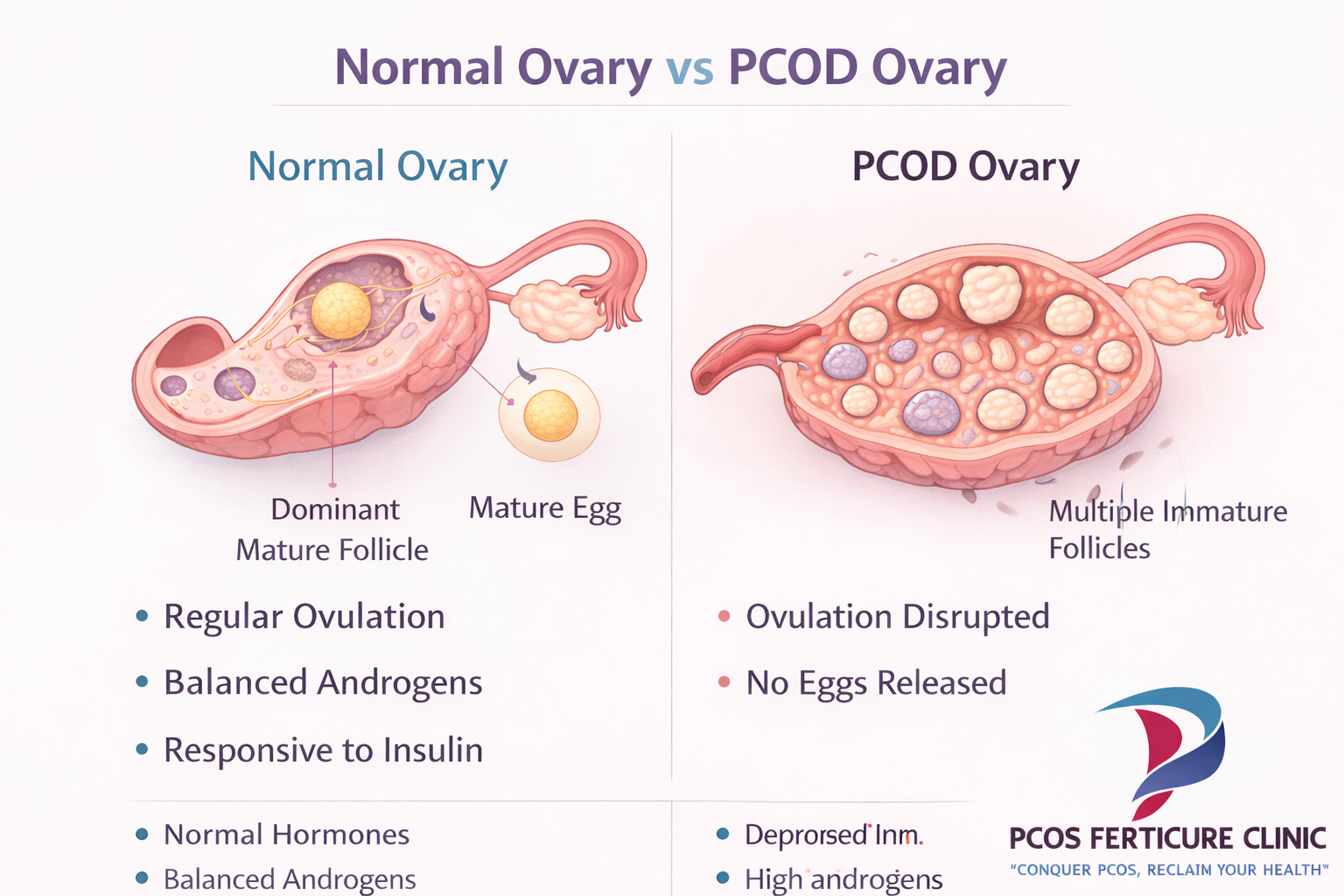
In a healthy menstrual cycle, the ovaries release one mature egg during ovulation. This process depends on precise hormonal communication between the brain, pituitary gland and ovaries. In Polycystic Ovary Disorder (PCOD), this hormonal coordination becomes disturbed. Instead of allowing one follicle to mature fully and release an egg, several follicles begin developing but stop growing midway. These partially developed follicles accumulate inside the ovary and appear as multiple small cyst-like structures on ultrasound.
Why Multiple Follicles Accumulate in the Ovary
These structures are often called “polycystic ovaries,” but they are not dangerous cysts in the surgical sense. They are simply immature follicles that did not complete their development. Because ovulation fails to occur regularly, menstrual cycles may become irregular, delayed or sometimes absent for several months.
Role of Androgen Hormones in PCOD
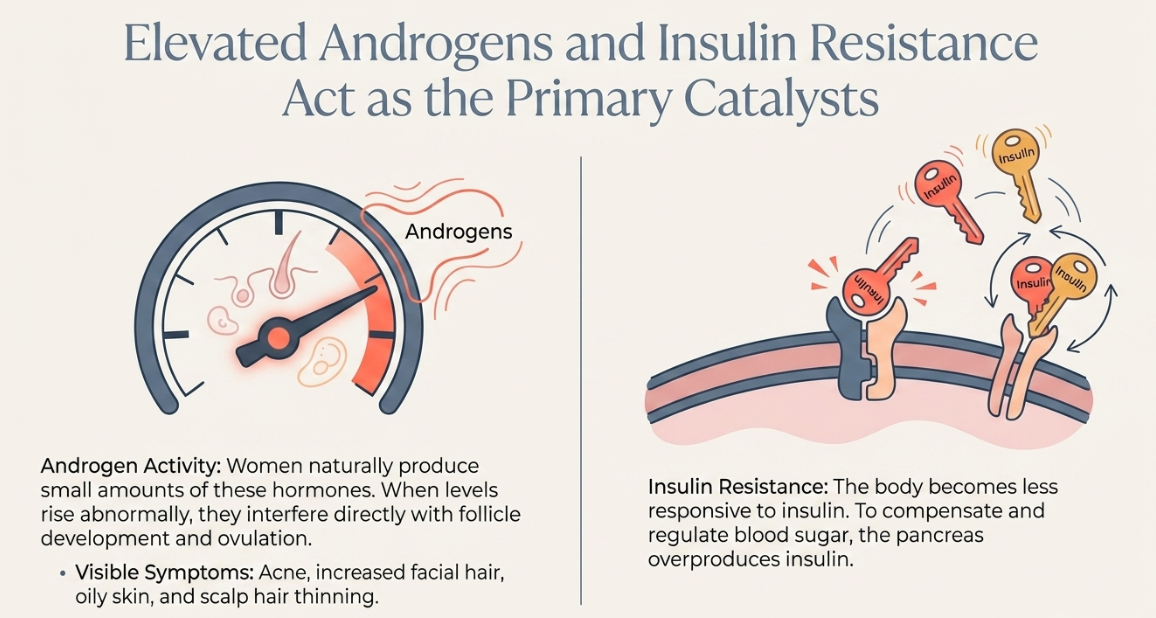
One of the main hormonal changes in PCOD involves increased androgen activity. Androgens are hormones that are typically associated with male characteristics, but women also produce small amounts of them naturally. When androgen levels rise above normal levels, they can interfere with follicle development and ovulation. This hormonal shift also contributes to visible symptoms such as acne, increased facial hair, scalp hair thinning and oily skin.
Insulin Resistance and Its Impact on Hormones
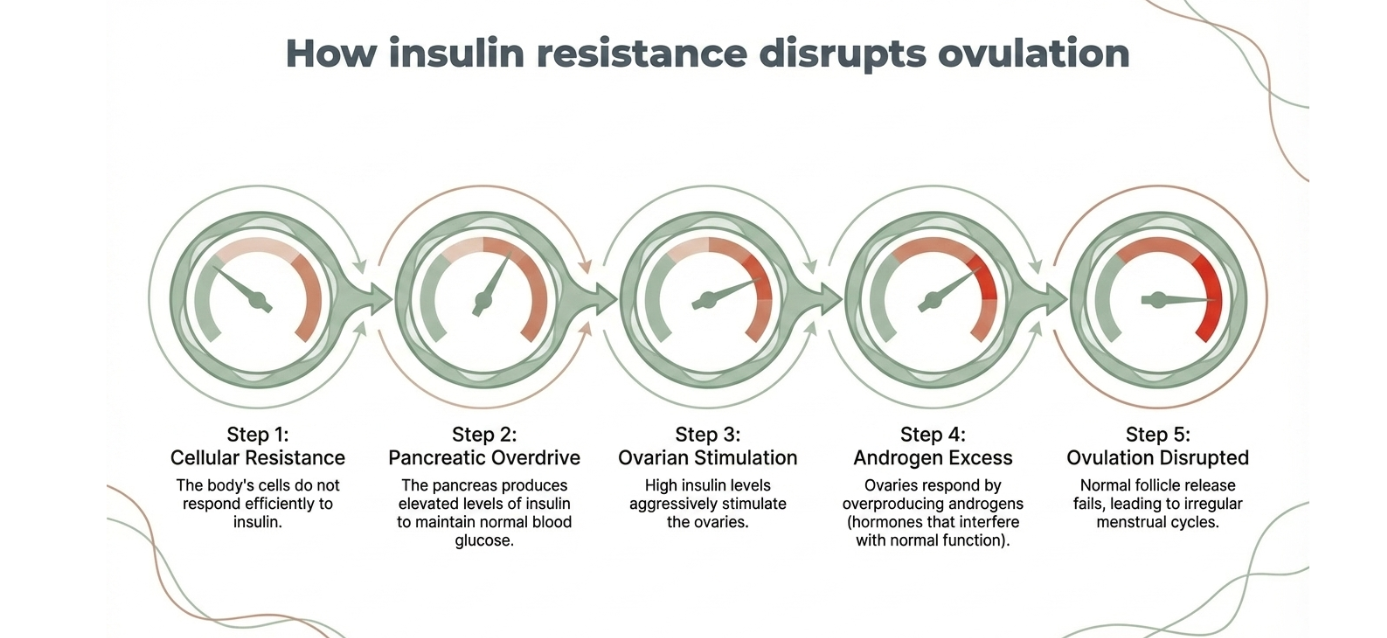
Another important factor associated with PCOD is insulin resistance. When the body becomes less responsive to insulin, the pancreas produces higher levels of insulin to regulate blood sugar. Elevated insulin levels can stimulate the ovaries to produce more androgens. This creates a cycle in which insulin resistance worsens hormonal imbalance, and hormonal imbalance further disrupts ovulation.
How Hormonal and Metabolic Changes Affect Health

Because of these interconnected mechanisms, PCOD affects both reproductive and metabolic health. Women may notice irregular periods, weight changes, acne or fertility concerns depending on how strongly these hormonal pathways are affected. If you want to understand how doctors confirm these hormonal patterns, our detailed guide on PCOS diagnosis explains the hormonal tests and ultrasound findings commonly used in clinical practice.
Understanding this hormonal mechanism is essential because it explains why PCOD management often focuses on restoring hormonal balance, improving insulin sensitivity and supporting healthy ovulation patterns. In the next section, we will clarify the commonly confused terms PCOD and PCOS and explain how they differ in medical discussions.
4. PCOD vs PCOS: Understanding the Difference

Why PCOD and PCOS Are Often Confused
Many women hear the terms PCOD and PCOS used interchangeably and assume they mean exactly the same thing. In everyday conversation, even patients, family members and sometimes healthcare providers may use these words as if they are identical. While they are closely related and share several features, they are not always understood in exactly the same way. Knowing the difference helps women better understand their diagnosis and treatment plan.
What Doctors Mean by PCOD
PCOD, or Polycystic Ovary Disorder, is commonly used to describe a condition in which the ovaries are affected by hormonal imbalance, leading to irregular ovulation, delayed periods and development of multiple immature follicles. In many women, the main concerns are irregular cycles, acne, facial hair growth, scalp hair thinning or weight gain. The focus is often on ovarian function and the symptoms directly linked to hormone imbalance.
How PCOS Is Considered a Broader Metabolic Condition
PCOS, or Polycystic Ovary Syndrome, is often considered the broader endocrine-metabolic syndrome. In addition to irregular ovulation and androgen imbalance, PCOS may have a stronger association with insulin resistance, metabolic dysfunction, inflammation and long-term health risks such as diabetes, metabolic syndrome and cardiovascular concerns. In other words, PCOS is generally discussed as a wider systemic condition rather than only an ovarian disorder.
That said, in real-world practice the distinction is not always rigid. A woman labeled as having PCOD may also show features commonly associated with PCOS, such as insulin resistance or significant metabolic difficulty. Similarly, a woman diagnosed with PCOS may mainly complain of irregular periods and acne. This is why many specialists focus less on the label alone and more on the individual pattern of symptoms, test results and treatment goals.
Why Doctors Focus More on Symptoms Than Labels
The most practical way to think about the difference is this: PCOD is often used in a narrower sense around ovarian dysfunction and hormonal imbalance, while PCOS is used in a broader sense that includes metabolic and endocrine disturbance. Both can affect menstrual health, skin, weight and fertility. Both may require lifestyle management, hormonal evaluation and long-term monitoring.
If you are still unsure how doctors evaluate these conditions, it may help to read our detailed guide on PCOS diagnosis, where we explain how menstrual history, ultrasound findings and blood tests are used together. If your concern is more about the practical side of symptom management, our guides on PCOS weight loss and PCOD diet chart can help you understand how metabolic support fits into treatment.
For most women, the key message is not to become overly anxious about whether the label is PCOD or PCOS. What matters more is understanding your ovulation pattern, hormone balance, metabolic status and long-term health risks. Once these are assessed properly, treatment can be personalized in a much more meaningful way.

5. Why PCOD Happens: Root Causes and Risk Factors
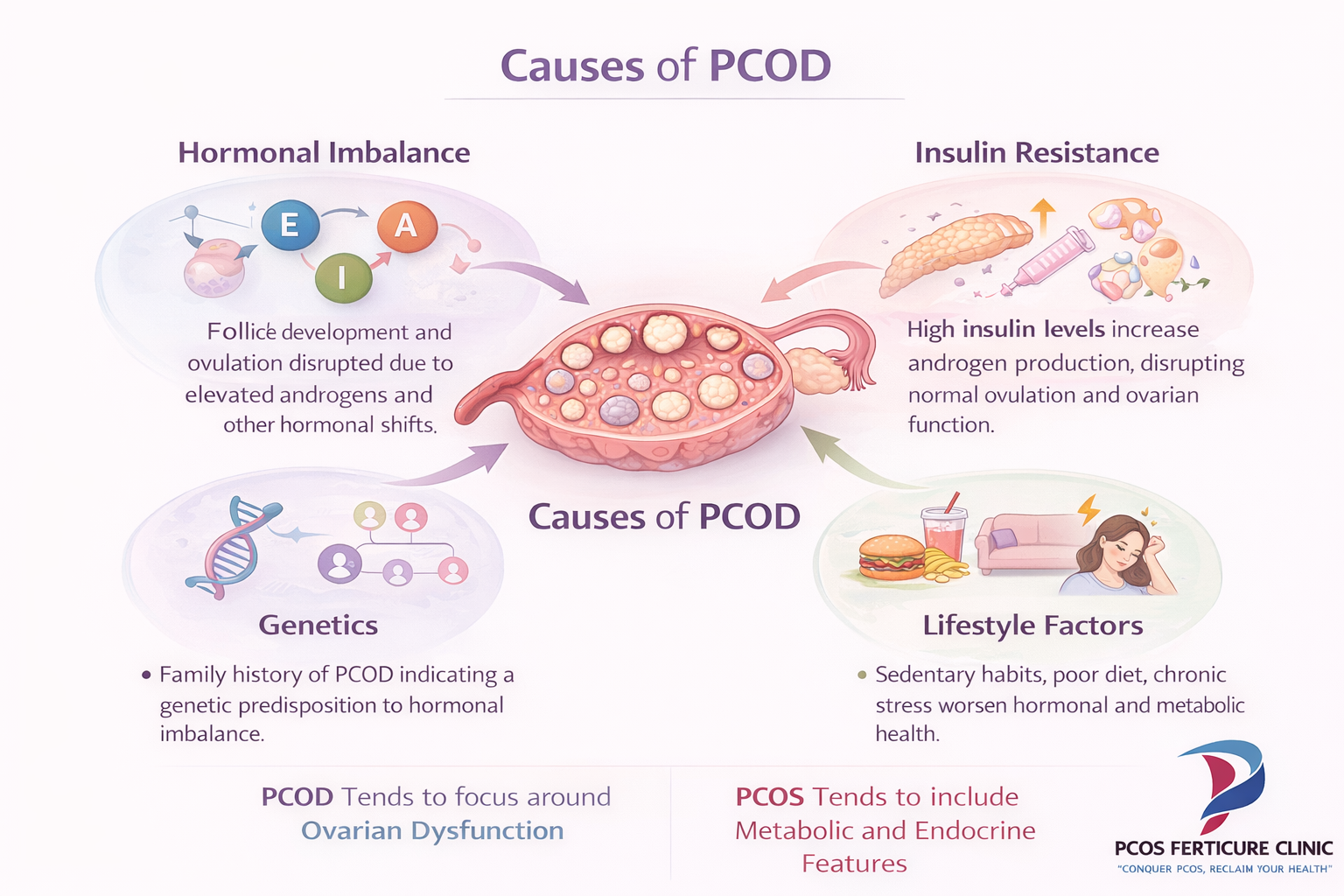
PCOD Is Usually Caused by Multiple Interacting Factors
Many women diagnosed with PCOD often ask the same question: why did this condition develop in the first place? Unlike certain diseases that have a single identifiable cause, PCOD develops due to a combination of hormonal, metabolic, genetic and lifestyle influences. These factors interact with each other over time and eventually disrupt the normal ovulation cycle.
Hormonal Imbalance and Ovulation Disruption
One of the primary contributors to PCOD is hormonal imbalance involving reproductive hormones. Normally, the ovaries respond to signals from the brain that regulate follicle growth and ovulation. However, when hormone levels become imbalanced, follicle development may stop prematurely and ovulation may not occur regularly. This disruption leads to irregular menstrual cycles and accumulation of immature follicles in the ovaries.
Insulin Resistance and Androgen Production
Another major factor involved in PCOD is insulin resistance. Insulin is the hormone responsible for regulating blood sugar levels. In insulin resistance, the body's cells do not respond efficiently to insulin, forcing the pancreas to produce higher levels of insulin to maintain normal blood glucose levels. Elevated insulin can stimulate the ovaries to produce more androgens, which are hormones that interfere with normal ovulation.
Genetic Susceptibility and Family History
Genetic predisposition also plays an important role. Many women with PCOD report that their mother, sister or close relatives have experienced irregular cycles, hormonal imbalance or fertility concerns. While there is no single gene responsible for PCOD, research suggests that inherited hormonal sensitivity and metabolic patterns may increase susceptibility to the condition.
Lifestyle and Environmental Risk Factors
Lifestyle factors can further amplify these underlying biological tendencies. Modern lifestyles characterized by high stress, irregular sleep patterns, sedentary habits and highly processed diets may influence hormonal balance and metabolic health. When these lifestyle factors interact with genetic predisposition and hormonal vulnerability, the likelihood of developing PCOD symptoms may increase.
Weight gain is sometimes discussed as a cause of PCOD, but the relationship is more complex. Hormonal imbalance in PCOD itself can make weight regulation difficult. Insulin resistance may encourage the body to store fat more easily, particularly around the abdomen. This is why many women notice that weight gain seems easier and weight loss feels more difficult compared with others. If you want to understand how weight management fits into PCOD care, our guide on PCOS weight loss explains the metabolic mechanisms involved and safe strategies to improve outcomes.
Dietary patterns also influence hormonal and metabolic balance. Foods that cause repeated spikes in blood sugar may worsen insulin resistance and contribute to hormonal fluctuation. Balanced nutrition that stabilizes blood glucose and supports metabolic health can be helpful for long-term symptom management. Our PCOD diet chart provides practical examples of meal patterns commonly recommended for women managing hormonal imbalance.
It is important to remember that PCOD develops gradually. It is not something a woman “causes” by doing something wrong. Instead, it reflects a complex interaction between hormones, metabolism, genetics and environment. Understanding these root causes helps women approach treatment with clarity and realistic expectations. In the next section, we will discuss the most common symptoms of PCOD and how they appear in everyday life.
6. Common Symptoms of PCOD
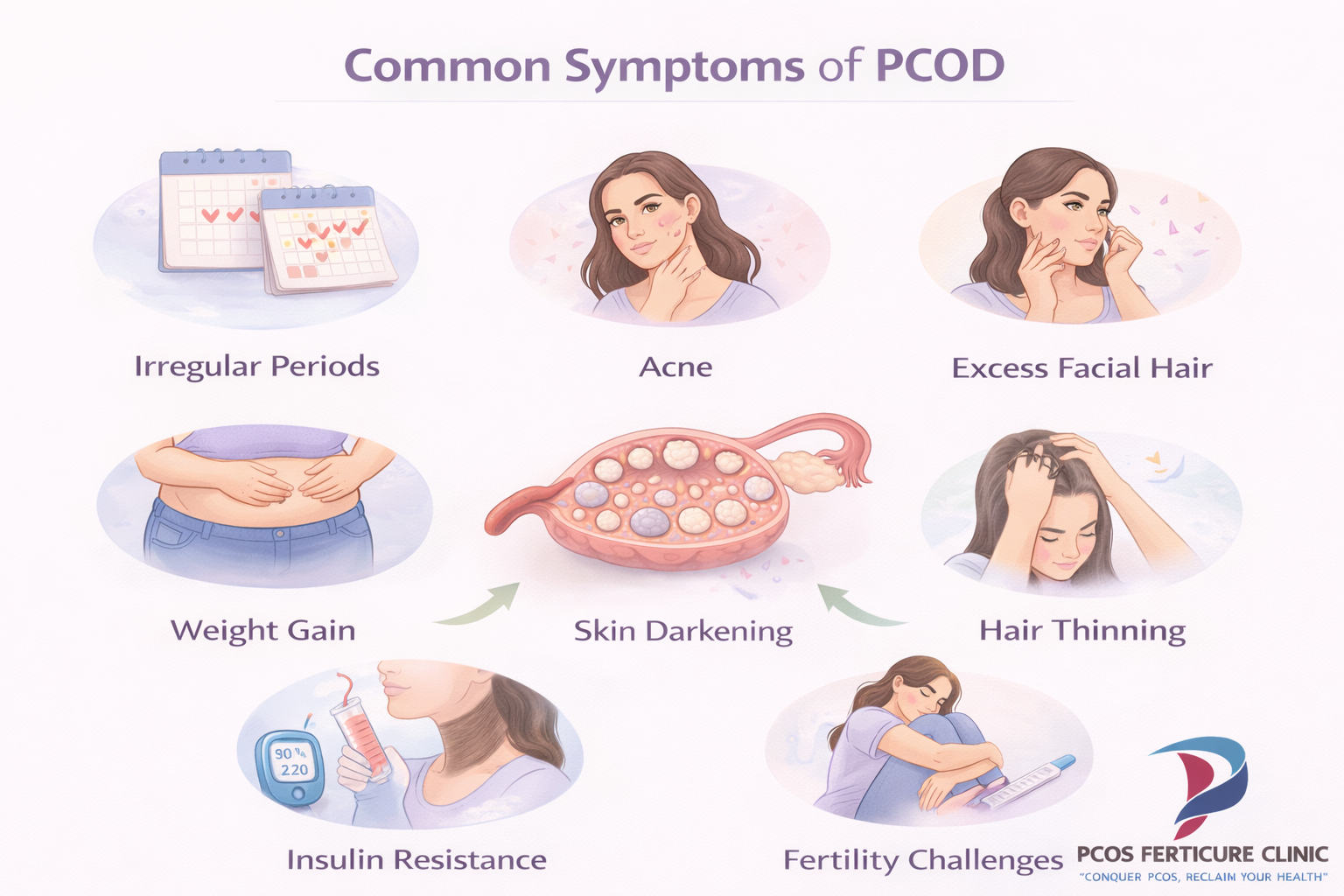
Why PCOD Symptoms Can Vary Between Women
PCOD can present in many different ways, which is one reason why it sometimes takes time for women to recognize the condition. Some women experience only mild symptoms, while others notice several changes occurring at the same time. These symptoms often develop gradually and may become more noticeable during late teenage years or early adulthood when hormonal patterns begin to stabilize.
Irregular Periods and Ovulation Problems
One of the most common signs of PCOD is irregular menstrual cycles. Women may experience delayed periods, cycles that occur several weeks apart or months when menstruation does not occur at all. This happens because ovulation does not occur regularly. When the ovary fails to release an egg consistently, the hormonal signals that regulate the menstrual cycle become disrupted.
Hormonal Acne and Skin Changes
Another frequently reported symptom is persistent acne or oily skin. Increased androgen activity can stimulate oil glands in the skin, leading to clogged pores and inflammatory acne. Unlike typical teenage acne, hormonal acne associated with PCOD often appears along the jawline, chin and lower face and may persist into adulthood.
Facial Hair Growth and Hair Thinning
Excess facial or body hair growth, known as hirsutism, may also occur due to elevated androgen levels. Women may notice increased hair growth on the chin, upper lip, chest or abdomen. At the same time, some women experience thinning hair on the scalp. This pattern occurs because androgen hormones affect hair follicles differently depending on the part of the body.
Weight Gain and Metabolic Symptoms
Weight gain or difficulty losing weight is another common concern associated with PCOD. Hormonal imbalance and insulin resistance may influence how the body stores fat and regulates metabolism. Many women report that weight gain seems easier even when their eating habits have not changed significantly. If weight management has been challenging, our guide on PCOS weight loss explains how hormonal and metabolic factors influence body weight in PCOD.
Fertility and Emotional Wellbeing
Some women also experience darkening of skin folds, particularly around the neck, underarms or inner thighs. This condition, known as acanthosis nigricans, may occur in association with insulin resistance. It is not harmful but may indicate underlying metabolic changes that should be evaluated.
Fertility concerns are another area where PCOD symptoms may become noticeable. Because ovulation occurs irregularly, it may take longer for some women to conceive naturally. However, it is important to understand that many women with PCOD successfully conceive with proper evaluation and treatment. You can learn more about this topic in our detailed guide on PCOS fertility treatment.
Beyond physical symptoms, hormonal imbalance may also influence emotional well-being. Some women report fatigue, mood fluctuations, anxiety or reduced motivation. These changes may be related to hormonal shifts, metabolic stress or the frustration of dealing with persistent symptoms.
Because PCOD symptoms vary widely, many women remain uncertain whether their experiences actually indicate hormonal imbalance. In the next section, you will be able to explore an interactive lifestyle and symptom evaluation tool that can help you understand whether your symptoms may be consistent with PCOD patterns.
7. PCOS Lifestyle Self-Evaluation Tool
Why Lifestyle Habits Influence PCOD Symptoms
Lifestyle patterns such as physical activity, diet quality, sleep habits and stress levels can significantly influence hormonal balance in PCOD. Regular exercise and balanced nutrition help improve insulin sensitivity, stabilize blood sugar and support ovulation patterns. Small daily habits often play an important role in long-term hormonal health.
Try the PCOS Lifestyle Self-Evaluation Tool
Understanding Your Lifestyle Score
This quick lifestyle evaluation gives a simple indication of whether current habits may support or worsen hormonal balance. The score is not a medical diagnosis but a starting point to understand whether exercise levels and sugar intake may be influencing PCOD symptoms. If your score suggests lifestyle improvements, gradual changes in diet, activity and sleep patterns can help improve metabolic health over time.
8. PCOS Lifestyle & Symptom Self-Evaluation Tool

Why PCOD Symptoms Are Sometimes Difficult to Recognize
Because PCOD symptoms can appear gradually and vary from one woman to another, many women remain unsure whether their experiences are related to hormonal imbalance or simply temporary lifestyle changes. Questions such as irregular cycles, acne, weight gain or mood fluctuations may occur independently at times, making it difficult to recognize a broader pattern.
Purpose of the PCOS Self-Assessment Tool
To help women better understand their symptoms, we have created a structured lifestyle and symptom evaluation tool. This interactive assessment helps identify common PCOD patterns by analyzing multiple factors such as menstrual health, metabolic indicators, hormonal symptoms and lifestyle habits. By answering a series of simple questions, you can gain insight into whether your symptoms may align with typical PCOD patterns.
The goal of this tool is not to replace medical diagnosis. Instead, it helps women become more aware of potential hormonal signals in their body and encourages them to seek proper evaluation when necessary. Many women discover through this type of structured self-evaluation that their symptoms follow recognizable hormonal patterns.
You can try the interactive evaluation here:
The assessment examines several areas that are commonly associated with PCOD:
- Menstrual cycle regularity and ovulation patterns
- Hormonal symptoms such as acne, hair growth and hair thinning
- Metabolic indicators including weight changes and insulin resistance signs
- Lifestyle factors such as sleep patterns, stress and activity levels
- Fertility-related concerns and reproductive health indicators
How the Assessment Results Help Guide Medical Consultation
Once the evaluation is completed, you will receive a structured interpretation of your responses that helps you understand potential hormonal risk patterns. Many women use this insight as a starting point for discussing symptoms with a gynecologist or endocrinologist.
After understanding your symptom profile, the next step is often lifestyle optimization. Nutrition and metabolic health play a crucial role in hormonal balance. In the next section we will explore how diet influences hormonal regulation and how structured meal planning can support women managing PCOD.
9. Lifestyle Changes That Help Manage PCOD

Why Lifestyle Changes Are Important in PCOD Management
While PCOD involves hormonal and metabolic changes, lifestyle habits play a powerful role in managing symptoms and improving long-term health. Many women notice that their symptoms fluctuate depending on diet, sleep patterns, stress levels and physical activity. Because of this connection, lifestyle management is often considered the foundation of PCOD treatment.
Exercise and Its Impact on Hormonal Balance
One of the most important lifestyle factors in PCOD is regular physical activity. Exercise helps improve insulin sensitivity, which means the body becomes more efficient at using insulin to regulate blood sugar. Better insulin sensitivity can reduce excess androgen production and support more stable hormonal patterns. Activities such as brisk walking, cycling, swimming or strength training can all contribute to metabolic balance when performed consistently.
Sleep Patterns and Hormonal Regulation
Sleep quality also has a strong influence on hormonal health. Irregular sleep schedules, chronic sleep deprivation and late-night screen exposure can disrupt hormonal rhythms in the body. When sleep patterns improve, many women notice better energy levels, improved metabolism and more stable mood patterns. Establishing a regular sleep schedule and limiting screen exposure before bedtime can be helpful for maintaining hormonal balance.
Stress Management and Cortisol Balance
Stress management is another important component of PCOD care. Chronic stress activates the body's cortisol response, which may influence insulin resistance and metabolic regulation. Relaxation practices such as yoga, breathing exercises, meditation or mindful movement can help stabilize stress hormones and support overall well-being.
Nutrition and Weight Management in PCOD
Nutrition is equally important when managing PCOD symptoms. Balanced meals that stabilize blood sugar levels can help reduce insulin spikes and support metabolic health. Whole grains, lean proteins, healthy fats, vegetables and fiber-rich foods often form the basis of dietary patterns recommended for women managing hormonal imbalance. If you would like practical examples of meal patterns designed for PCOD, you can explore our PCOD diet chart, which provides structured meal ideas commonly used to support hormonal balance.
Weight management can also play a supportive role for some women with PCOD, particularly when insulin resistance is present. Even modest improvements in metabolic health may help restore more regular ovulation patterns in certain cases. Our detailed guide on PCOS weight loss explains why weight management can be difficult in PCOD and what strategies are considered safe and sustainable.
It is important to remember that lifestyle management is not about achieving perfection. Small, consistent improvements in daily habits often produce meaningful results over time. When lifestyle support is combined with appropriate medical guidance, many women experience improvement in menstrual regularity, metabolic health and overall well-being.
In the next section, we will explore how nutrition specifically influences hormonal regulation and how structured diet planning can support women managing PCOD.
10. Weekly PCOS Lifestyle Planner
Why Structured Weekly Planning Helps Manage PCOD
Managing PCOD often requires consistency rather than drastic changes. Weekly planning helps organize lifestyle habits such as exercise, meal timing, stress management and sleep routines. When these habits are planned in advance, it becomes easier to maintain metabolic balance and support hormonal regulation over time.
Generate Your Personalized PCOS Lifestyle Plan
Understanding and Using Your Weekly Lifestyle Plan
The generated weekly plan provides a simple framework for building consistent health habits. It may include suggested exercise routines, nutritional focus areas and lifestyle practices that support hormonal balance. The goal is not perfection but gradual improvement in daily habits that influence metabolic and reproductive health.
11. PCOD Diet Planning and Hormonal Nutrition

Why Nutrition Plays a Key Role in PCOD Management
Nutrition plays a central role in managing PCOD because food directly influences metabolic health, insulin levels and hormonal balance. Many women with PCOD experience insulin resistance, which means the body has difficulty using insulin efficiently to regulate blood sugar levels. When insulin levels remain elevated for long periods, the ovaries may produce higher levels of androgens. These hormonal shifts can disrupt ovulation and contribute to symptoms such as irregular periods, acne and weight gain.
Blood Sugar Balance and Insulin Regulation
Because of this connection between insulin and hormones, dietary patterns that stabilize blood sugar are often recommended for women managing PCOD. Meals that contain balanced proportions of complex carbohydrates, lean protein, healthy fats and fiber tend to produce more gradual blood sugar responses. This helps reduce insulin spikes and supports metabolic stability.
Low Glycemic Foods That Support Hormonal Balance
Low glycemic foods are particularly helpful for maintaining steady blood sugar levels. These foods digest more slowly and prevent rapid glucose fluctuations. Examples include whole grains such as oats and brown rice, legumes such as lentils and chickpeas, and fiber-rich vegetables such as spinach, broccoli and carrots. Including protein sources such as eggs, fish, tofu or lean poultry alongside carbohydrates can further stabilize blood sugar responses.
Healthy Fats and Anti-Inflammatory Nutrition
Healthy fats also play an important role in hormonal regulation. Foods such as nuts, seeds, olive oil and avocados contain beneficial fatty acids that support metabolic health and may help reduce inflammation. Inflammation has been increasingly recognized as a contributing factor in hormonal imbalance and metabolic dysfunction associated with PCOD.
Highly processed foods, sugary beverages and refined carbohydrates can worsen insulin resistance and contribute to metabolic fluctuations. While occasional indulgence is normal, consistently consuming foods that rapidly elevate blood sugar may intensify hormonal instability over time. This is why many PCOD dietary plans emphasize whole foods, fiber-rich meals and balanced nutrition rather than extreme dieting approaches.
Practical Diet Planning for Women Managing PCOD
Structured meal planning can make it easier to follow a hormone-supportive diet in daily life. Our detailed guide on PCOD diet chart provides practical meal examples designed to support hormonal balance and metabolic stability. The guide includes meal combinations commonly used in Indian diets while keeping glycemic balance and nutritional diversity in mind.
Dietary changes do not need to be drastic to produce benefits. Small adjustments such as improving meal balance, increasing fiber intake and reducing refined sugar consumption can gradually support hormonal health. When combined with regular physical activity and adequate sleep, these nutritional strategies may contribute significantly to long-term PCOD management.
In the next section, we will explore how weight management interacts with PCOD and why many women find weight loss more challenging when hormonal imbalance and insulin resistance are present.
12. PCOS Friendly Food Explorer
Understanding Food Choices in PCOD
Food choices play an important role in supporting hormonal balance and metabolic health in women managing PCOD. Certain foods help stabilize blood sugar levels, reduce inflammation and support healthy insulin response. Other foods may cause rapid blood sugar fluctuations that can worsen insulin resistance and hormonal imbalance. Understanding these differences allows women to build meals that support long-term metabolic stability rather than short-term dietary restriction.
Explore PCOS Friendly Food Categories
The food explorer below groups common foods into three practical categories: foods that are highly supportive for hormonal balance, foods that can be consumed in moderation and foods that are better limited in daily diets. These categories are not strict rules but general nutritional guidelines commonly used in PCOD lifestyle management.
Using Food Categories to Plan Balanced Meals
The goal of these food categories is not to eliminate foods completely but to guide balanced meal planning. A PCOD friendly plate usually combines fiber rich carbohydrates, lean protein and healthy fats. This combination slows digestion, stabilizes blood sugar and supports hormonal balance. By using supportive foods more frequently and limiting high glycemic foods, many women find it easier to maintain consistent energy levels and metabolic health.
13. PCOD and Weight Gain: Why Weight Loss Feels Difficult

Why Weight Gain Is Common in PCOD
One of the most frustrating experiences reported by many women with PCOD is the difficulty in managing body weight. Some women notice gradual weight gain despite maintaining eating habits similar to others around them. Others may attempt multiple diet plans and exercise routines but see only minimal changes in body weight. Understanding why this happens requires looking at the metabolic changes associated with PCOD.
Insulin Resistance and Fat Storage
A key factor involved in PCOD-related weight gain is insulin resistance. When the body's cells become less responsive to insulin, the pancreas compensates by producing higher levels of insulin to regulate blood sugar. Elevated insulin levels encourage the body to store energy as fat, particularly in the abdominal region. This metabolic pattern makes it easier for the body to gain weight and more difficult to lose it.
Hormonal Imbalance and Appetite Regulation
Hormonal imbalance also contributes to changes in appetite regulation and energy metabolism. Increased androgen levels may influence how the body distributes fat and how efficiently calories are used for energy. Some women with PCOD report experiencing stronger hunger signals or reduced satiety after meals, which can further complicate weight management.
Lifestyle Factors That Influence Metabolism
Another factor is the interaction between metabolism and lifestyle patterns. When hormonal imbalance affects energy levels, women may feel more fatigued and less motivated to maintain consistent exercise routines. Sleep disturbances, stress and irregular schedules can also influence metabolic hormones that regulate appetite and fat storage.
It is important to understand that weight gain in PCOD is not simply a result of willpower or discipline. The metabolic environment created by insulin resistance and hormonal imbalance can make weight management more challenging compared with individuals who do not have these hormonal patterns. This is why weight loss strategies for PCOD often focus on improving metabolic health rather than relying on extreme calorie restriction.
Sustainable Weight Management Strategies for PCOD
Structured approaches that combine balanced nutrition, strength training, cardiovascular activity and improved sleep patterns often produce better outcomes than short-term dieting. Even small improvements in insulin sensitivity may help restore hormonal balance and support more regular ovulation patterns.
If you would like a step-by-step approach designed specifically for hormonal metabolism, you can explore our interactive guide on PCOS weight loss planning. This guide explains how metabolism, insulin resistance and lifestyle patterns interact and provides practical strategies to support gradual and sustainable progress.
In the next section, we will explore how PCOD can influence fertility and pregnancy planning, and what treatment approaches may help women who are trying to conceive.
14. PCOD and Fertility: Can Women With PCOD Get Pregnant?

Fertility Concerns in Women With PCOD
One of the most common concerns among women diagnosed with PCOD is whether the condition will affect their ability to conceive. Because PCOD can disrupt ovulation and cause irregular menstrual cycles, many women worry that pregnancy may not be possible. However, it is important to understand that many women with PCOD successfully conceive with appropriate medical guidance and lifestyle support.
The Role of Ovulation in Pregnancy
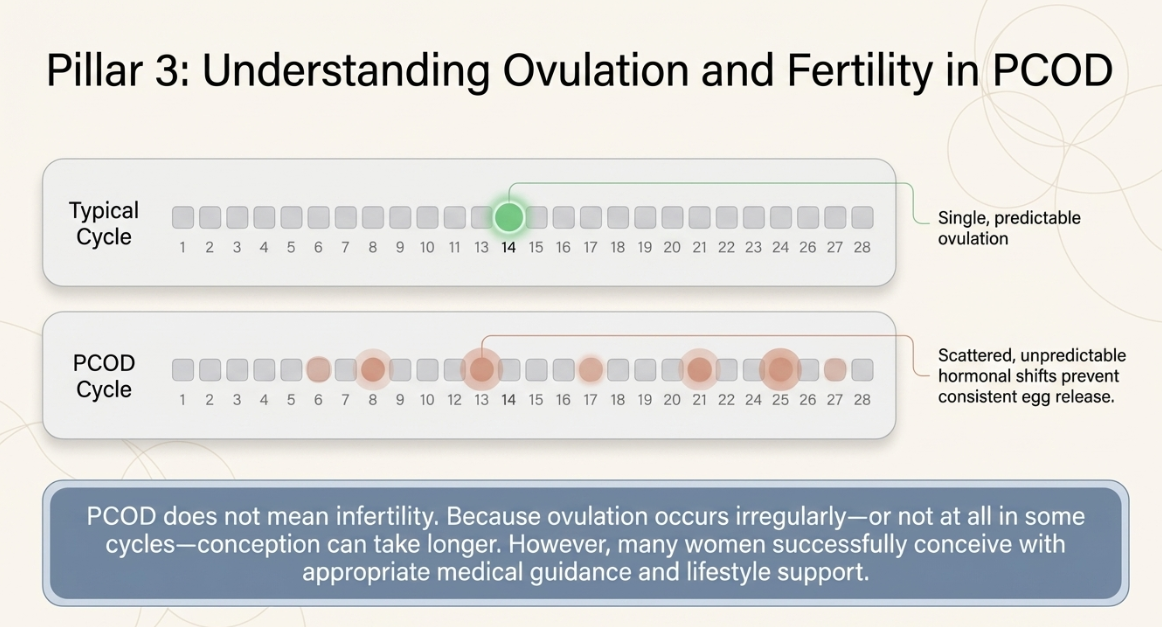
Ovulation plays a central role in fertility. During a normal menstrual cycle, the ovary releases a mature egg that can be fertilized by sperm. In PCOD, ovulation may occur irregularly or may not occur in some cycles. This irregular ovulation is the main reason why conception can sometimes take longer for women with PCOD compared with those who have regular cycles.
Lifestyle Factors That Can Improve Fertility
Fortunately, modern reproductive medicine offers several effective approaches for improving ovulation patterns. Lifestyle interventions such as improving nutrition, increasing physical activity and managing insulin resistance can often restore ovulation in some women. Even modest improvements in metabolic health may positively influence reproductive hormones.
Medical Treatments That Support Ovulation
When lifestyle adjustments alone are not sufficient, doctors may recommend medications that stimulate ovulation. These treatments help the ovary release an egg at the appropriate time during the menstrual cycle. With proper monitoring, many women are able to achieve successful pregnancy using these approaches.
Pregnancy Outcomes in Women With PCOD
It is also important to understand that PCOD does not affect every woman in the same way. Some women with PCOD ovulate occasionally and may conceive naturally without medical intervention. Others may require fertility support depending on how strongly hormonal imbalance affects their ovulation cycle.
If you are planning pregnancy and have concerns related to PCOD, early evaluation can be helpful. Hormonal testing, ultrasound examination and cycle tracking can provide valuable information about ovulation patterns and reproductive health. You can learn more about treatment options in our guide on PCOS fertility treatment, which explains how doctors approach fertility management for women with hormonal imbalance.
It is reassuring to remember that PCOD does not mean infertility. With proper diagnosis, lifestyle support and appropriate medical treatment when needed, many women with PCOD successfully conceive and deliver healthy pregnancies.
In the next section, we will explore medical treatment options commonly used to manage PCOD symptoms and improve hormonal balance.
15. Medical Treatment Options for PCOD

Individualized Treatment Planning in PCOD
Treatment for PCOD is usually personalized based on a woman's symptoms, hormonal profile and reproductive goals. Because PCOD affects both hormonal and metabolic systems, treatment strategies often combine lifestyle adjustments with medical therapies that address specific symptoms such as irregular periods, acne, insulin resistance or fertility concerns.
One of the most common goals of treatment is restoring regular menstrual cycles. Hormonal medications may sometimes be prescribed to regulate menstrual cycles and stabilize hormone levels. These medications help balance estrogen and progesterone patterns and reduce excessive androgen activity. Regulating cycles can also help protect the uterine lining and improve overall reproductive health.
Managing Insulin Resistance
Another important treatment focus involves addressing insulin resistance. When insulin levels remain elevated for long periods, they can worsen hormonal imbalance and contribute to symptoms such as weight gain, acne and irregular ovulation. In some cases, doctors may recommend medications that improve insulin sensitivity. These medications help the body utilize insulin more effectively and may support improved metabolic and hormonal balance.
Treatments for Acne and Excess Hair Growth
For women experiencing acne or excessive hair growth, treatment may include medications that reduce androgen effects on the skin and hair follicles. Dermatological care and hormonal therapy may work together to improve these symptoms gradually over time.
Fertility-Focused Medical Treatments
When fertility is a priority, doctors may recommend ovulation induction therapies. These treatments stimulate the ovary to release an egg during the menstrual cycle, increasing the chances of conception. Ovulation induction is often carefully monitored using ultrasound and hormone testing to ensure safe and effective treatment.
Role of Lifestyle in Long-Term PCOD Management
It is important to remember that PCOD treatment is not limited to medications alone. Lifestyle interventions such as improving diet, increasing physical activity and managing stress remain essential components of long-term care. Many women experience significant improvement in symptoms when medical treatment is combined with metabolic and lifestyle support.
If you would like to understand how diagnosis guides treatment planning, our detailed guide on PCOS diagnosis explains how hormonal evaluation and ultrasound findings help doctors choose appropriate treatment strategies.
Because PCOD affects each woman differently, regular follow-up with a qualified gynecologist or endocrinologist is important. With proper monitoring and individualized care, most women are able to manage symptoms effectively and maintain good reproductive and metabolic health.
16. Scientific Research and Medical Evidence on PCOD

Polycystic Ovary Syndrome (PCOS) and Polycystic Ovarian Disease (PCOD) have been widely studied by medical researchers across the world. Over the past two decades, scientific research has helped doctors understand the hormonal, metabolic and genetic factors involved in this condition. These studies have also helped shape modern diagnostic guidelines and treatment strategies used by gynecologists and endocrinologists today.
According to the World Health Organization (WHO), PCOS is one of the most common hormonal disorders affecting women of reproductive age. It is estimated to affect approximately 8-13 percent of women globally, although many cases remain undiagnosed. This highlights the importance of awareness, early evaluation and appropriate medical guidance.
Research published in PubMed indexed journals has shown that insulin resistance plays a central role in many cases of PCOS. Studies demonstrate that elevated insulin levels may stimulate the ovaries to produce higher levels of androgens, which can disrupt ovulation and contribute to symptoms such as acne, irregular periods and excessive hair growth.
The Endocrine Society has published clinical practice guidelines for the diagnosis and management of PCOS. These guidelines emphasize the importance of a comprehensive evaluation that includes menstrual history, hormonal testing, metabolic assessment and ultrasound examination. This holistic approach helps doctors differentiate PCOS from other hormonal disorders and design appropriate treatment strategies.
Several studies published in leading medical journals such as The Lancet and Human Reproduction have also explored the long-term health implications associated with PCOS. Researchers have observed that women with PCOS may have an increased risk of metabolic conditions such as insulin resistance, type 2 diabetes and cardiovascular risk factors if hormonal imbalance remains untreated for long periods.
At the same time, research has also demonstrated that lifestyle interventions can significantly improve metabolic and reproductive outcomes. Clinical studies show that improving diet quality, maintaining regular physical activity and managing body weight may help restore ovulation in some women and reduce metabolic complications associated with PCOS.
Scientific evidence therefore supports a comprehensive treatment approach that combines medical care with lifestyle support. Early diagnosis, personalized treatment planning and long-term follow-up play a critical role in improving health outcomes for women affected by PCOD.
If you would like to understand how PCOS is diagnosed clinically, you can read our detailed explanation on PCOS diagnosis and evaluation. You may also explore our PCOS diet chart and PCOS weight loss guide to understand how lifestyle strategies support hormonal balance.
17. When Should You See a Doctor for PCOD?

Many women experience occasional hormonal fluctuations during their reproductive years. However, when certain symptoms begin to appear regularly or interfere with daily life, it may be important to seek medical evaluation. Early consultation with a qualified gynecologist can help identify whether these symptoms are related to PCOD or another hormonal condition.
One of the most common reasons women seek medical advice is irregular menstrual cycles. If menstrual periods occur very infrequently, become unpredictable or stop for several months at a time, it may indicate an underlying hormonal imbalance. Regular evaluation can help identify the cause and guide appropriate treatment.
Persistent acne, excessive facial hair growth or hair thinning on the scalp may also indicate elevated androgen levels. These symptoms can sometimes be dismissed as cosmetic concerns, but they may reflect deeper hormonal changes that require medical attention.
Weight gain that occurs despite maintaining a balanced diet and physical activity may also warrant evaluation. In many cases, insulin resistance plays a role in PCOD-related weight changes, and early management can help prevent long-term metabolic complications.
Women who are planning pregnancy but experiencing difficulty conceiving may also benefit from medical evaluation. Because PCOD can affect ovulation patterns, identifying the condition early allows doctors to recommend treatment strategies that improve fertility outcomes.
A comprehensive medical evaluation typically includes a detailed health history, hormonal blood tests and ultrasound examination of the ovaries. These investigations help doctors understand the hormonal patterns involved and develop a personalized treatment plan.
If you are experiencing symptoms related to PCOD, seeking professional medical guidance can help you understand your condition and begin appropriate treatment. You can also start with our PCOS lifestyle self-evaluation tool to assess common symptoms and hormonal health patterns.
You may also explore our detailed guides on PCOS diet planning and PCOS weight loss strategies to understand how lifestyle changes support hormonal balance.
Remember that PCOD is a manageable condition. With proper diagnosis, lifestyle guidance and medical treatment when necessary, most women are able to restore hormonal balance, manage symptoms effectively and maintain long-term reproductive and metabolic health.
18. Long-Term Health Risks of Untreated PCOD

PCOD is often recognized because of symptoms such as irregular menstrual cycles, acne or weight gain. However, beyond these visible symptoms, untreated hormonal imbalance may also influence long-term metabolic and reproductive health. This is why early diagnosis and appropriate management play an important role in protecting long-term wellbeing.
One of the most significant metabolic concerns associated with PCOD is insulin resistance. When the body’s cells become less responsive to insulin, blood sugar regulation becomes less efficient. Over time this metabolic pattern may increase the risk of developing prediabetes or type 2 diabetes if lifestyle and hormonal factors remain unmanaged.
Hormonal imbalance may also influence cardiovascular risk factors. Some women with PCOD may develop elevated cholesterol levels, increased abdominal fat distribution or changes in blood pressure regulation. While these risks vary from person to person, regular medical monitoring helps identify these patterns early and guide preventive care.
Reproductive health may also be affected if ovulation remains irregular for prolonged periods. Women who experience persistent ovulation irregularities may face challenges when planning pregnancy. However, with early evaluation and appropriate treatment strategies, many women with PCOD are able to restore ovulation patterns and successfully conceive.
Another concern related to long-term hormonal imbalance involves the uterine lining. When menstrual cycles occur infrequently, the uterine lining may remain exposed to estrogen without the balancing effect of progesterone. Medical evaluation helps ensure that menstrual cycles are regulated and the uterine lining remains healthy.
It is important to understand that these risks do not occur in every individual with PCOD. Many women manage their condition effectively through a combination of lifestyle adjustments and medical care. Maintaining balanced nutrition, regular physical activity and healthy sleep patterns can significantly improve metabolic health and hormonal balance.
If you are concerned about symptoms related to PCOD, you can begin by exploring our PCOS lifestyle self-evaluation tool. You may also read our guides on PCOS diet planning and PCOS weight loss strategies to understand how lifestyle changes support hormonal health.
Early awareness, regular monitoring and appropriate treatment allow most women with PCOD to maintain good reproductive, metabolic and overall health throughout their lives.
19. Frequently Asked Questions About PCOD
PCOD (Polycystic Ovarian Disease) is a hormonal condition in which the ovaries produce higher levels of androgens. This imbalance can interfere with ovulation and lead to symptoms such as irregular periods, acne, weight gain and fertility concerns.
PCOD refers to ovarian dysfunction with multiple immature follicles, while PCOS is considered a broader endocrine syndrome involving metabolic changes such as insulin resistance and hormonal imbalance.
PCOD may develop due to hormonal imbalance, insulin resistance, genetic predisposition and lifestyle factors such as sedentary habits and poor dietary patterns.
Early symptoms may include irregular periods, acne, facial hair growth, weight gain, hair thinning and difficulty losing weight.
PCOD can affect ovulation patterns which may make conception more difficult, but many women conceive naturally or with appropriate treatment.
Yes. Many women with PCOD conceive successfully, especially when hormonal balance and ovulation patterns improve with treatment.
Insulin resistance associated with PCOD can promote fat storage and make weight loss more difficult.
Even modest weight loss may improve insulin sensitivity and help regulate menstrual cycles.
A diet rich in fiber, lean protein, healthy fats and low glycemic carbohydrates can support metabolic health.
Strength training, walking, yoga and aerobic exercise improve insulin sensitivity and metabolic health.
Doctors diagnose PCOD through menstrual history, hormonal blood tests and ultrasound examination.
Tests may include hormone levels such as LH, FSH, testosterone, insulin and pelvic ultrasound.
Yes. Elevated androgen levels may increase oil production in the skin leading to acne.
Some women experience hair thinning due to hormonal imbalance affecting hair follicles.
Insulin resistance in PCOD may increase the risk of developing type 2 diabetes if unmanaged.
Hormonal imbalance and physical symptoms may contribute to anxiety, mood changes and stress in some individuals.
Yes. Lifestyle modifications such as diet, exercise and sleep improvement can significantly improve symptoms.
If you have persistent irregular periods, severe acne, unexplained weight gain or difficulty conceiving.
With proper treatment and lifestyle care, most women manage PCOD effectively long term.
PCOD may influence metabolic health, fertility and hormonal balance, but proper management greatly reduces risks.



